What is Coronary Angiography?
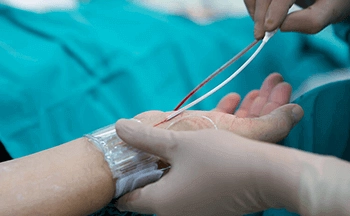
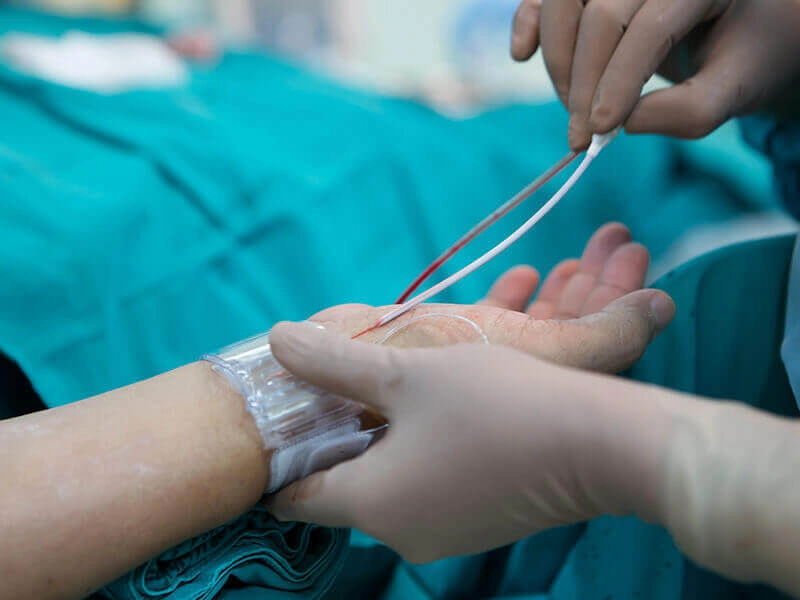
Coronary angiography is a procedure in which a special X-ray of the heart’s arteries (the coronary arteries) is taken to see if they are narrowed or blocked. It is an important test, used when the doctor suspects a coronary heart disease. The procedure is performed under a local anesthetic and a catheter (a long thin tube) is put into an artery in the groin, or at the inside of the elbow or near the wrist. The catheter is moved up the inside of the artery until it reaches the heart. A special dye is then injected into the coronary arteries and X-rays are taken. The X-ray image (a ‘coronary angiogram’) gives detailed information about the state of the heart and coronary arteries.
When is a Coronary Angiography needed?
Coronary angiography is considered as the gold standard investigation for detecting coronary artery disease and is done under different circumstances:
-
Sometimes it is done in patients who present with a heart attack,
-
or in those who have a positive treadmill,
-
or in patients who present with either chest pain or breathlessness during exercise,
-
or if the patient is suspected to have coronary heart disease.
The doctor may recommend the test if the patient has chest pain that is suspected to be caused by narrowed coronary arteries, or if the doctor wants to assess the degree of narrowing in the coronary arteries.
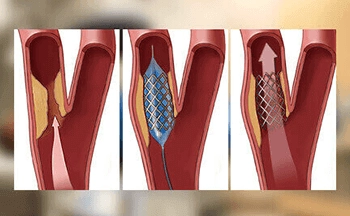
Coronary Angioplasty will further help to see if the patient can benefit from a procedure such as angioplasty or bypass surgery, to relieve the symptoms and reduce the risk of further heart problems like a heart attack.
Are there any risks involved?
As with many medical tests, there are some risks involved, rarely any serious problems develop. Most people have no trouble, and the benefits usually far outweigh the risks. The patient can always discuss with the doctor any questions or concerns they may have about coronary angiography.
Earlier Coronary angiography was done through the groin route, whereas nowadays it is done through the wrist route. When doing it through the groin route, the major complication is primarily related to the access site bleeding. Because it is a large artery in the groin, the bleeding complications can sometimes be quite nasty, often necessitating blood transfusions or surgical procedures to close the hole or the bleed in the artery. Sometimes because of the clotting in the leg artery, the patient may also require blood thinners or procedures to remove the clot.
These complications related to the access site have now been substantially reduced by now doing the coronary angiography through the wrist route. Because it is a small artery, very easily accessible and present against the bone. The bleeding complications are eliminated and there is no risk of losing the pulse because there are 2 parallel arteries running in the wrist that take care of the circulation to the hand. Therefore in going through the wrist artery, there is no risk of losing the wrist artery.
Coronary angiography can rarely induce any heart-related complications like heart rhythm disorders or heart attacks. Also, there is a very rare possibility of a stroke because we are catheterizing the aorta from where some plaque might get disturbed and go into the brain artery and cause strokes. Fortunately, these complications are very rare.
Other complications are related to the use of the contrast medium which is used to opacify the artery during Coronary angiography. These are iodinated contrasts but sometimes may cause some mild allergies like itching or wheals or rashes etc. Very rarely serious allergic reactions like bronchospasm or severe anaphylactic reactions which are life-threatening can occur but are very uncommon. And whenever such reactions occur, they occur in the Cath Lab, thus can be easily managed because all the emergency equipment is available.
The other important complication that one needs to be very careful is in the very elderly and in those who have preexisting kidney diseases, where the radiographic contrasts can cause contrast-induced nephropathy leading to the deterioration of the kidney function. Therefore, these complications can be avoided by limiting the amount of contrast and aggressively hydrating the patient after the procedure, choosing a kidney safe contrast along with careful patient selection.
So when we chose a Coronary angiography in the right way for the right reasons and perform it safely, it is a very safe procedure. However, one should always be aware of the possible complications and be ready to manage them.
How is a Coronary Angiography performed?
Coronary angiography is done in special laboratories (‘cath-labs’) that look like operating theatres. The patient is taken there on a trolley, or in a wheelchair, and asked to lie on a narrow table, which will be moved from side to side during the test. The patient is connected to a machine that will monitor the heartbeat continuously. Many people have a small needle put into a vein in the back of one hand to allow medicines to be given during the test.
The doctor will inject a local anesthetic into the groin, arm or wrist (where the catheter is to be inserted) and if the arm is used, a small cut will be made. The catheter will be inserted into the main artery at that point.
The catheter is moved through the main blood vessel of the body (the aorta), to the beginning of the coronary arteries of the heart. Its progress is watched via X-rays shown on a monitor. Most people will not feel any pain or sensation during the test. As there are no nerves inside the arteries, the patient will not feel the movement of catheters through the body.
When the catheter is in place, a small amount of X-ray dye will be injected into it. X-rays will be taken as the dye travels through the coronary arteries. These X-rays will be shown on a monitor and recorded on a computer. Different catheters are needed to study the various arteries. One will be removed and the next introduced through the same place in the groin or arm.
Some people have nausea or chest discomfort when the dye is injected, but this does not last long. A larger injection of dye is given if the heart muscle is to be examined. This may give a warm feeling in the upper chest first, then over the rest of the body. The feeling may last for about 10 to 15 seconds.
The test will take about 30 to 40 minutes. When the test has been completed, the catheter will be removed and pressure is applied to the area where it was inserted. Patients can be then shifted to the ward or recovery area to rest in bed for at least four hours. In most circumstances, the patient will be allowed to go home after four to six hours. Some people may need to stay in the hospital longer so that their symptoms can be monitored further. The X-ray dye passes through the kidneys and is excreted in the urine.