Neuromodulation is the procedure that involves direct stimulation of the nervous system with electrical signals or direct administration of medicines into the nervous system for therapeutic purposes. It modulates the activity of target cells in the brain or the nervous system at specific locations in the body, delivering mild electrical stimulation or drugs in order to relieve pain or restore function. The technique is primarily used for the treatment of unmanageable chronic pain and/or movement disorders.
The most common neuromodulation therapies depending on the type of disorder include:
1. Spinal cord stimulation to treat chronic neuropathic pain;
2. Deep brain stimulation for movement disorders.
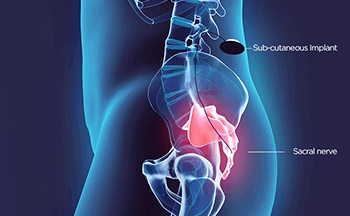
3. Sacral nerve stimulation for pelvic pain, bladder and motion problems disorders (incontinence / retention)
4. Spinal cord stimulation for ischemic disorders such as angina and peripheral vascular disease.
Persistent nerve pain or functional problems of bladder are better regulated than lifelong medications which usually have various side-effects. A gentle dose of electric current delivered to the precisely identified appropriate nerves helps to regulate abnormal nerve function.
Two major factors that contribute significantly in patient selection for the stimulation therapy are:
-
Patients should be willing to undergo the trial therapy before committing to permanent battery implantation – A trial lead is precisely placed at an appropriate nerve providing an opportunity to try the effect of treatment before committing to permanent implantation of pulse generator battery.
-
Reversibility without permanent damage – Neurostimulation is a non-ablative (no deliberate nerve destruction) and completely reversible therapy.
Sacral Nerve Stimulation
What is sacral nerve stimulation?
Sacral nerve stimulation is also known as Pelvic Neuromodulation has proven to be quite a useful treatment option for chronic dysfunction of the urinary, bowel and pelvic floor. In pelvic neuromodulation, the sacral nerve that controls the bladder, bowel and pelvic floor and the muscles related to their function, is stimulated with mild electrical pulses. The stimulation enables the person to perceive the sensation of bladder fullness and the desire to empty the bladder, spontaneously and completely.
How does sacral nerve stimulation work?
The muscles in the pelvic area, such as the pelvic floor, urethral sphincters, bladder and anal sphincter are all controlled by the brain through nerves that run from the sacral area. Our sensations, such as fullness in the bladder or rectum, are also relayed to the brain via these nerve routes.
SNM works by activating or inhibiting the urinary tract reflexes, by delivering mild electrical impulses to the sacral nerve that serves the lower urinary tract. Besides the local stimulation, neuromodulation also influences the higher centers of bladder control in the brain (known as pontine micturition center).
When is sacral nerve stimulation indicated?
SNM is indicated in patients with chronic urinary retention, voiding dysfunction, bowel dysfunction and chronic pain syndromes. In patients with chronic urinary retention, the only known forms of treatment are clean intermittent self-catheterization (CISC) or indwelling supra-pubic/transurethral catheters. At times CISC can be a painful and traumatic process, and SNM offers an effective therapeutic alternative.
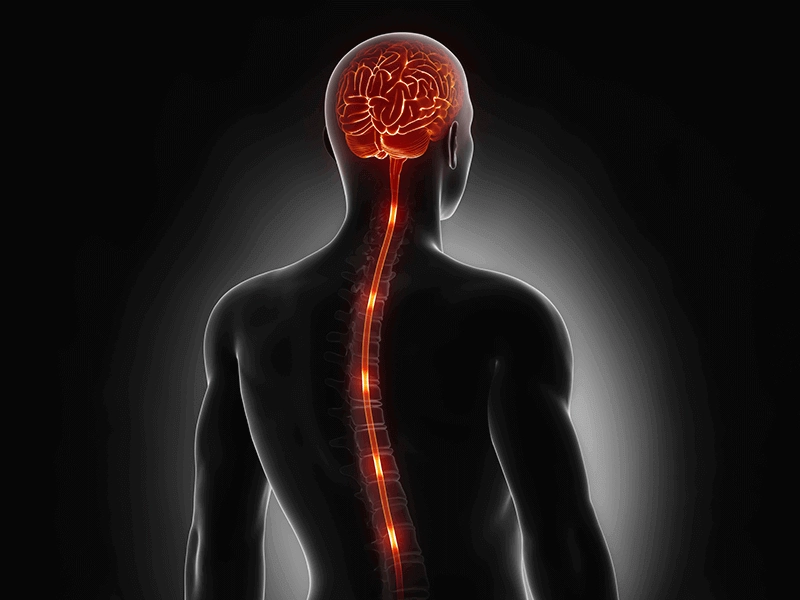
Spinal Cord Stimulation
This common form of neuromodulation involves using a device to deliver electrical current in therapeutic doses to the spinal cord to disrupt pain signals from the spinal cord to the brain, converting them to a more pleasant tingling sensation. This has been proven a safe and effective therapeutic approach for managing chronic pain of the arms and legs, neck and back often after spine surgery, or for other neuropathic conditions. This is indicated in persistent nerve pain conditions like:
1. Post-Spine surgery nerve pain
2. Diabetic Neuropathy
3. Complex Regional pain syndrome
4. Post herpetic neuralgia
5. Post Amputation Phantom pain
6. Peripheral Vascular (Circulation) disease
7. Severe Angina in spite of CABG / Stenting
What does neuromodulation involve?
Neuromodulation involves the surgical implantation of three components just like a pacemaker implant in the heart:
1. A lead – special insulated wires with an electrode at the tip that delivers mild electrical pulses to the affected area
2. Extension wires – connect the electrodes to the neurostimulator
3. A Pulse Generator – which is a small electronic device implanted under the skin, leaving no device hanging out of the body. This can be programmed to deliver the right current using a sophisticated remote. The stimulator sends mild electrical pulses via insulated leads to targeted areas of the spinal cord, the nerves or brain to block the transmission of signals that either cause pain or bladder control problems.
Implantation of a neuromodulating stimulator is a procedure which takes around 3 to 6 hours (in one or two stages) and is usually done under a local anesthesia by a skilled and experienced interventional pain physician.
What are the benefits for neuromodulation?
Neuromodulation therapies improve peoples’ lives by providing an alternative line of treatment to long-term drug therapy and giving symptomatic relief from persistent or chronic conditions. Such treatment options are significant especially when existing drugs are not proving to be effective or are resulting in problems like tolerance development, addiction, adverse side-effects or toxicity.
What are the side effects of these treatments?
Similar to any other procedure, neuromodulation also has some minor easily manageable complications which are specific to the technique, therapy and disease. The majority of issues are easily dealt with adjustments in the implanted hardware. Fortunately, serious complications are extremely rare, making it a procedure with a very high safety profile.