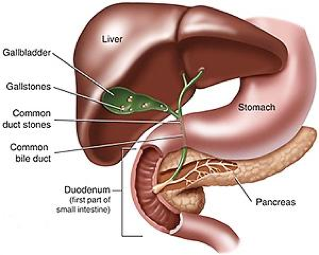
The Gallbladder is a small pouch that is a storehouse for excess bile. It is just below the liver and joins the main bile draining ducts.
When we eat, the gallbladder contracts to expel bile into the intestine for the digestion of fats.
.png)
Gallstones or cholelithiasis (from the Greek chol (bile)- lith (stone)- iasis (process)) are formed due to cholesterol-forming stones in the gallbladder.
.png)
No particular reason, but it occurs more in females, people with diabetes; those with a family history of gallstones; people who are overweight, obese, or undergo rapid weight loss; and those taking cholesterol-lowering drugs. With age the incidence of gallstones increases.
.png)
If you are symptomatic, then you need surgery. It’s your body’s way of telling you that your gallbladder is not functioning properly. Asymptomatic gallbladder stones are generally not operated on. Any complication is heralded by some symptoms.

Symptoms can range from vague bloating, a feeling of indigestion, or pain.

Pain is usually on the right side of the upper abdomen or in the middle. It is usually severe but can vary in intensity. Pain can be over the right shoulder too (referred pain).

In patients with diabetes, these tend to be very easily ignored because of lesser perception of pain - till some serious complication sets in.
Complications can be pus forming in the gallbladder, perforation of the gallbladder, obstructive jaundice (stone slipping from the gallbladder into the main bile passage and obstructing the bile flow), pancreatitis (inflammation of the pancreas).
The gold standard treatment for symptomatic gallstones is laparoscopic cholecystectomy (keyhole gallbladder removal) . We have emphasized on ”removal” because in a gallstone problem the gallbladder needs to be removed unlike kidney stones, where only the stones are removed and not the kidney.
Once gallstones give trouble, the gallbladder becomes inflamed and subsequently non-functional. Hence retaining it serves no purpose. Additionally – retaining a diseased gallbladder can predispose to further severe complications like pus formation/cancer developing.
Hence a simple surgery is done– where the connection between the gallbladder and the main bile draining ducts is clipped and cut and the gallbladder is removed from one of the keyholes made for surgery. The integrity of the main biliary tract is maintained, and only the diseased reservoir is removed.
In case of severe inflammation around the gallbladder or difficulty in performing a surgery then the doctor may leave a small part of the gallbladder behind while removing the majority of the gallbladder with the stones. This small part of the gallbladder is closed off or left open depending on the inflammation and a drain is placed to the area, which is subsequently removed
.png)
At Sakra, we have an expert team of surgeons that has conducted more than 1500 Gall Bladder (GB) surgeries in 5 years with zero risk in bile duct surgeries. Our surgeons are experienced in handling difficult GB surgeries by laparoscopy.
Dr. Sadiq Sikora is renowned in the field of Bellary surgery in India. He has conducted several training courses for safe cholecystectomy across India. He is a member of the National & International expert group, which has developed guidelines for safe cholecystectomy surgery in India and across the world.
Facilities available at Sakra World Hospital for cholecystectomy include:
.png)
• 3D laparoscopy: Better vision and precision of surgery
• ICG guided surgery: The use of ICG with a specialized camera enables us to see the bile duct during the surgery and thereby preventing damage and injury to the bile duct.
We have well-equipped modular OT with facilities for Intraoperative Cholangiogram or Endoscopic retrograde cholangiography (ERC).
Fortunately, the gallbladder is an organ people can live without. Your liver produces enough bile to digest a normal diet. Once the gallbladder is removed, bile flows out of the liver through the hepatic ducts into the common bile duct and directly into the small intestine, instead of being stored in the gallbladder. There are no specific dietary restrictions or lifestyle changes after gallbladder surgery.
It takes around 1 and ½ - 2 hours for regular gallbladder surgery. The time can be more in case of a complicated case. The time of stay in the OT complex will be more. It includes wheeling in time, signing in, anesthesia induction, surgery, and recovery out of anesthesia. The patient will be monitored for 2-3 hours in the recovery area, before shifting the patient back to the room.
We would like to request the family members to make themselves comfortable in the waiting room/ward till the doctor calls them to talk about how the procedure went.
After the surgery, you can start having liquids after 6-7 hours of recovery from anesthesia and gradually increase your intake.
You may have some pain, soreness in the right upper abdomen and around the umbilicus. There may be some right shoulder pain that subsides in 24-48 hours. You can also experience a sore throat sensation which usually subsides in 24-48 hours. These kinds of pain are easily manageable with some IV painkillers and should keep you pretty comfortable.
You are admitted the previous night of the surgery or on the morning of the surgery. Most patients get discharged the following morning of the surgery.
There are no sutures to be removed. A follow-up visit will be scheduled to see the wound healing and remove the dressings.
Immediately the next day. We will put waterproof dressings, hence taking a bath without soiling the sutures is possible.
On discharge some discomfort in the abdominal wounds maybe there which will need medications. Activities can be increased as per your comfort level.
Rejoining work will depend on the patient’s comfort level and type of work involved, but usually, after 5-7 days, normal activities can be resumed.
There are no specific restrictions/precautions after the surgery. There are no diet modifications needed to be made after gall bladder removal. No restrictions on activities either apart from the immediate post-operative period of recovery.
If the LFT is deranged (abnormal liver function tests) then based on the pattern we decide if an MRCP/ EUS is required.
If a CBD stone is found, you will need an ERCP – endoscopic retrieval of the CBD stone to clear the bile passage +/- stenting. The stent is for a brief duration and will be removed after the gallbladder surgery
Pain similar to preoperative pain can recur after surgery if a small stone gets slipped into the bile duct and has not been picked up in the preoperative evaluation. If this happens, further tests will be done as deemed necessary and then ERCP can be done to remove it. Surgery is not required again.
If for any reason, you have undergone a subtotal removal of the gallbladder, there is a small possibility that you may develop stones in the remnant gallbladder stump later. If this is detected, then a completion cholecystectomy can be performed.
Generally, the procedure and recovery are uneventful. The most common post-operative events can be some
-Pain/discomfort at the operative port sites.
-Infection
Rarely (in 0.5-0.7% of cases) there may be an intra-abdominal collection due to bile leak from some adjacent structures. This may require a drainage/subsequent surgery as decided by the surgeon.
